It is generally accepted that cartilage is not able to heal or regenerate itself after injury or through wear and tear, leading to the development of osteoarthritis. But there is a body of evidence emerging that challenges this view.
Recent studies show evidence of cartilage regeneration following a surgical procedure called joint distraction. A research team from the Centre for Osteoarthritis Pathogenesis, Versus Arthritis within the Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Sciences (NDORMS) set out, in collaboration with partners in the Netherlands, to investigate whether there were molecular changes within the environment of the knee joint that could explain the repair.
The team studied a group of 20 individuals with osteoarthritis undergoing knee joint distraction, an intervention that uses an external frame fixed to both sides of the joint to gradually pull apart the knee by 5mm over 6 weeks. A benefit of the treatment, which is not yet offered in the UK, is that it takes pressure off the joint while enabling the patient to continue to walk on the leg. Knee joint distraction has previously been shown in clinical studies by the Netherlands group not only to lead to sustained improvements in knee symptoms but also to repair cartilage as measured by magnetic resonance imaging.
"It's something that goes against the dogma because people think that once the cartilage is gone that's it," said Fiona Watt, Associate Professor at NDORMS. "We were interested to know whether this intervention was changing the joint environment to promote cartilage regrowth, and if we could measure markers which might represent repair pathways. Identifying such pathways might help us to develop new treatments to prevent or delay knee arthroplasty or to treat osteoarthritis in other joints in the future, as well as understanding how this particular intervention brings about benefit."
A small sample of joint fluid was taken from each patient when the knee distraction frame was fitted, at the mid-point of distraction, and at six weeks, the point at which the distractor was removed. Patients were followed for a year in total and their osteoarthritis symptoms assessed. The team looked for changes in a panel of ten markers, previously identified as important in the response to joint injury and in repair, to determine whether any changes in the fluid could be linked to response to intervention and clinical improvement.
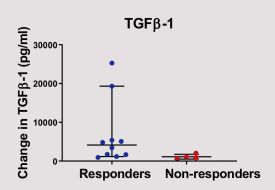
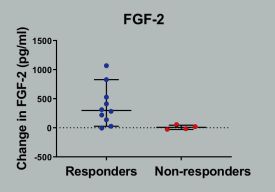
"Several markers changed with distraction, but two markers, FGF2 and TGFß, showed a significant increase in the joint during distraction and predicted a good clinical outcome," said Professor Tonia Vincent, Director of the Centre for OA Pathogenesis at NDORMS. "Both of these are growth factors that are associated with cartilage repair in laboratory studies. Although ours was a small exploratory study, it shows that the biology in the joint changes rapidly when mechanical stress is altered and this likely facilitates cartilage repair. Identifying the molecules that drive the intrinsic power of cartilage to repair may help us to identify new molecular treatments for osteoarthritis.
Caroline Aylott, Head of Research Delivery at Versus Arthritis says, “This work by our Centre for Osteoarthritis Pathogenesis is important in helping us to understand the biological processes at work when the body is trying to repair damage to cartilage. By understanding the chemical signals involved, we may, in the future be able to develop treatments to help repair cartilage and reduce the need for joint replacements.”
Published in Osteoarthritis Research Society International, the study was supported by Versus Arthritis, ReumaNederlands, the Dutch Arthritis Society, and by the NIHR Oxford Biomedical Research Centre (BRC).


 ©
Shutterstock
©
Shutterstock